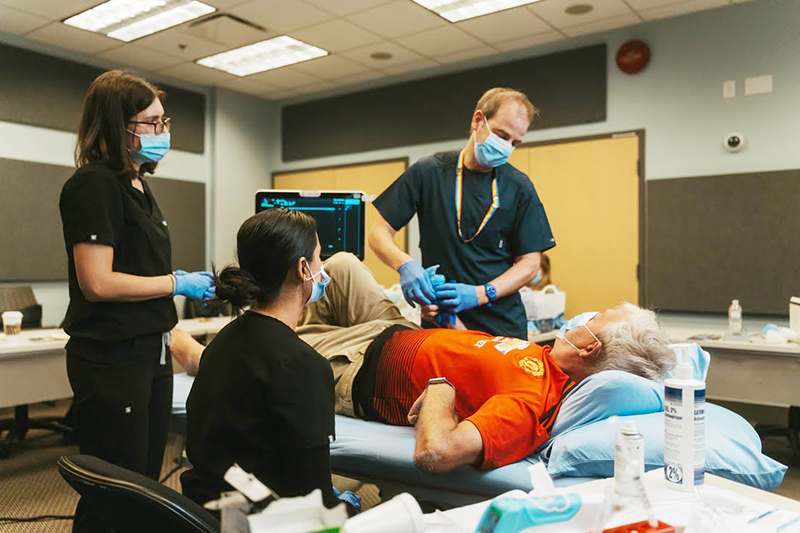
Victoria Treatment Being Used to Help Patients Regain Mobility
 Cryoneurolysis is an ultrasound-guided treatment kills targeted contracted motor nerves to treat spasticity (paralysis) with few ill effects.
Cryoneurolysis is an ultrasound-guided treatment kills targeted contracted motor nerves to treat spasticity (paralysis) with few ill effects.
It’s a treatment using cryotherapy guided by non-invasive ultrasound developed by Psychiatrist Dr. Paul Winston, interventional anesthesiologist Dr. Daniel Vincent and plastic surgeon Dr. Emily Krauss.
Reprint of an article written by Cindy E. Harnett appeared in the Sunday November 2nd 2025 Times/Colonist
As quickly as a brain aneurysm changed Sarah Millard’s life at age 21, a team of Victoria doctors changed it back — two decades later.
It started on a Monday morning in June 2005. Millard was back at her parents’ home in Victoria, two courses shy of completing a degree in economics and French at the University of Guelph in Ontario, when she fell out of bed.
She thought she had gotten caught up in her sheets and then realized she had momentarily lost control of her limbs.
An ambulance took her to Victoria General Hospital where she was diagnosed as having had a transient ischemic attack, a TIA, caused by a brief blockage of blood flow to the brain that produces symptoms similar to a stroke.
She regained her mobility, but a diagnostic angiogram detected a large aneurysm — “a bit of a time bomb in my brain,” Millard said.
Within four days, she was flown to Vancouver General Hospital, where she underwent brain surgery.
It didn’t go as planned and Millard had a stroke.
“I woke up after surgery, and half my body was paralyzed,” said Millard, who would spend months in GF Strong Rehabilitation Centre in Vancouver, and many more months in out-patient rehabilitation at Victoria General Hospital.
With a positive attitude and support from family and friends, Millard relearned everything when using her left side — how to write, eat, exercise, walk and run.
Finding a job with a disability was initially hard, she said, but almost a decade after her surgery, she had earned her Certified General Accountant’s qualification and set herself up professionally.
She still couldn’t fully raise her arm, open her hand or lift her right foot. She accepted her disability but hid it.
Her life would dramatically change, however, when she met Victoria physiatrist Dr. Paul Winston last year at a Dance Victoria event.
Dr. Paul Winston and “Spasticity”
From Winston, she learned about “spasticity,” a neurological disorder caused by injuries to the brain or spinal cord that result in abnormal muscle tightness, common after a stroke and brain injuries, or as a result of cerebral palsy or multiple sclerosis.
We have motor nerves that are always relaxing and contracting as directed by the brain. When that signal gets mixed up, some motor nerves remain in a contracted, stiff position.
“Doctors had never used that term, spasticity, with me — it was always the word ‘paralyzed,’ not spasticity, so it was not something I looked into treatment for,” said Millard.
Winston, medical director of rehabilitation and transitions for Island Health, said that in about 2017, he became “fed up with the unsatisfactory results and expense of botulinum treatments, such as Botox, or opioids used to treat pain and improve mobility”.
He was interested in a new kind of surgery being done on nerves in Europe, where surgeons were cutting motor nerves to treat spasticity. But only so many could be cut at a time.
Inspired, Winston and his colleagues — interventional anesthesiologist Dr. Daniel Vincent and plastic surgeon Dr. Emily Krauss — came up with something of a twist: using cryotherapy guided by non-invasive ultrasound.
The technique would draw upon Vincent’s idea to freeze and kill affected motor nerves controlling mobility, Winston’s clinical research skills in ultrasound, and Krauss’s surgical knowledge of nerves and how to repair skin stretched over rigid limbs.
The treatment, called cryoneurolysis, involves an ultrasound-guided probe and the use of a special one-time-use needle to freeze and destroy overactive motor nerves. At −88 C, the treatment kills targeted contracted motor nerves but not tissue.
It eliminates surgery and surgical scars and greatly increases the number of nerves treated.
The ultrasound-guided therapy targeting motor nerves was not being done anywhere else, said Winston. He found one case report from a physician who tried a similar treatment on a patient’s leg and a study started in 2014 that was never published.
But nobody was doing it in clinical practice anywhere in the world that we know of,” Winston said.
Winston and his colleagues started treating their first patients in 2018 and the positive results were immediate. They ramped up to a full service starting in 2021 and have treated more than 1,000 patients since then. With the clinic at Victoria General Hospital operating four days a week, they are now in a position to do 400 procedures a year.
Successful Outcomes from Cryoneurolysis Treatment
Winston said successfully treated patients in the community, and in hospital and long-term care homes, include stroke survivors who are now able to unlock their arms, fists and legs from frozen positions. “It’s mind-blowing,” Winston said.
One success was a bride who was able to walk down the aisle without fear of falling, along with children with cerebral palsy who can now run, throw a ball or get rid of their leg braces.
The first paper the physicians published in 2023 on this technique showed that of 113 patients treated, 96.7 per cent of the nerves treated showed improvement with no adverse events. The remaining patients had pain symptoms due to insufficient freezing, which could be treated or were resolved in a few months.
Winston said patients are not just going home from hospital, “they are going back to work. They no longer need their caregivers.”
Some are able to play piano or climb stairs again or even run, he said.
Patients see the best results if treated immediately after injury or the onset of the condition. Some are so severely injured they might not be able to regain their full mobility with treatment, but might regain enough to make life easier, he said.
Winston said there are few other surgeries or treatments where patients walk out an hour later considerably better.
“Patients leave crying and running or walking and moving dramatically different,” said Winston, who also conducts research on spasticity, spinal cord and nerve injury, and complex regional pain syndrome, through the Victoria Peripheral Nerve and Spasticity Clinic at Victoria General Hospital.
“We get patients to walk stairs and they haven’t walked stairs in 20 years.”
Over the years, the team has built an international curriculum “on how to relax every muscle in the body by attacking its motor nerves,” said Winston, who teaches the procedure to physicians around the globe.
“There’s now about 70 centres all over the world using the treatment we invented here in Victoria,” said Winston, adding clinics in North America and Europe, including at Harvard, Yale and Oxford universities, offer “the made-in-Victoria” treatment. “It’s quite amazing.”
Winston said the clinic’s goal is to see every patient who has a neurological disorder treated immediately — every elderly person in hospital who’s having difficulty walking or moving because of contracted muscles caused by a neurological disorder and every child with spasticity.
He said the handheld ultrasound probe used in the procedure was designed for an outpatient clinic, but B.C. rules require the procedure to be done in a hospital.
Island Health funds 32 treatments for neurological patients per month, while the province continues to audit the program to gather evidence to determine if it should be provided province-wide.
Winston said the program is cost efficient. For example, he uses a $630 needle for the treatment. Botulinum, such as Botox, used in other treatments costs about $2,000 four times a year. “It’s dramatically cheaper,” Winston said of his procedure.
Over the years, the clinic, whose partners have published more than 30 peer-reviewed papers, has raised close to $1 million from donors, industry partners, research grants and other awards which supports its co-op students and research assistants. A fundraising event was held Oct. 26 at Elements Casino.
Winston said that given the demand, the clinic would be greatly aided by more co-op students, a nurse and a physiotherapist.
Millard, now 41, said she had “massive results” from her May 2024 treatment, which was topped up in May this year.
She said she will never again take for granted the joy of being able to perform simple tasks such as holding an ice cream cone, using a pair of scissors, hanging laundry or combing her hair, and cried “happy tears” on and off for weeks.
A nurse who saw her leave the hospital and was unaware of her treatment asked if she had just had a cast removed. Millard said it was a perfect metaphor for her feeling of breaking free from mental and physical constraints that imprisoned her.
“I had dealt with these paralyzing symptoms every day for 19 years, and it took up so much space in my life.”
While she has always practised Pilates in her house, she’s now training to become an instructor, on a mission to help people of all ages and abilities move. “I was living my life as a disabled person, that was what I had come around to accept, but now I’m not,” said Millard.
“It’s just so freeing being able to keep writing my own story and not being restricted by something that happened to me.